Introduction
In the realm of foot health, one condition that can significantly impact mobility and overall well-being is posterior tibial tendonitis. This ailment involves inflammation and irritation of the posterior tibial tendon, a crucial structure that supports the arch of the foot. When affected, individuals may experience pain, swelling, and difficulty performing daily activities.
Recognizing the importance of seeking appropriate treatment for timely recovery is essential. Ignoring or neglecting posterior tibial tendonitis can lead to further complications, such as flatfoot deformity or chronic instability. Therefore, it is crucial to address this condition promptly and effectively to restore foot health and prevent long-term issues.
The purpose of this article is to provide readers with insights into the various treatment options available for posterior tibial tendonitis. By understanding these options, individuals can make informed decisions about their course of action and take the necessary steps toward a successful recovery. Whether it be conservative approaches like rest, compression, and elevation or more advanced treatments such as orthotics, physical therapy, or even surgical interventions, this article aims to shed light on effective methods to alleviate symptoms and improve foot function.
By delving into the treatment options for posterior tibial tendonitis, readers will gain valuable knowledge that can guide them in seeking appropriate care. Remember, timely intervention and the right treatment approach are vital in managing posterior tibial tendonitis and restoring foot health and mobility.
Understanding Posterior Tibial Tendonitis
Definition and Causes of Posterior Tibial Tendonitis
Posterior tibial tendonitis refers to the inflammation of the posterior tibial tendon, which runs along the inner side of the ankle and foot. This condition commonly occurs due to overuse or repetitive stress on the tendon, leading to microtears and subsequent inflammation. Factors that can contribute to the development of posterior tibial tendonitis include excessive running or jumping, improper footwear, obesity, and biomechanical abnormalities like flat feet or high arches.
Symptoms and Common Signs of Posterior Tibial Tendonitis
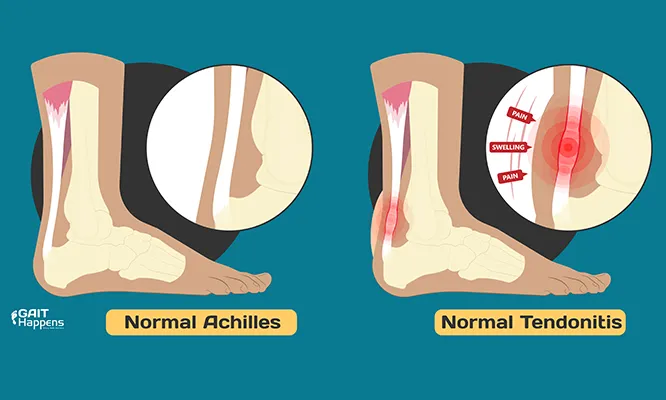
Recognizing the symptoms and signs of posterior tibial tendonitis is crucial for early detection and appropriate treatment. Individuals with this condition often experience pain, swelling, and tenderness along the inner ankle and arch of the foot. The pain may worsen with activity, especially during walking or running. In advanced cases, individuals may notice a flattening of the arch, leading to an altered foot posture.

Importance of Early Diagnosis and Prompt Treatment
Timely diagnosis and treatment play a vital role in managing posterior tibial tendonitis effectively. Early intervention can help prevent the condition from progressing and minimize the risk of long-term complications. Ignoring the symptoms or delaying treatment may lead to further tendon damage, foot deformities, and chronic instability. Seeking medical attention and diagnosis from a healthcare professional specialized in foot and ankle conditions is crucial to receive an accurate assessment and initiating appropriate treatment promptly.
There are 4 stages of Posterior Tibialis Tendon Dysfunction. This is why it is mandatory to have your foot assessed sooner than later if you are experiencing pain. The sooner the correct diagnosis is made, the sooner the appropriate rehabilitation can be implemented.
In the first 2 stages, the foot is still mobile and typically can be strengthened. These strength programs should not only focus on foot strength but also hip and core strength. If left untreated, stages 3 and 4 can occur. At these stages, the foot is becoming more rigid, and the successful prognosis decreases. Orthotics and even surgery may be recommended at these stages.
Physical Therapy Exercises and Stretches
Physical therapy exercises and stretches are essential components of conservative treatment for posterior tibial tendonitis. These exercises aim to strengthen the posterior tibial tendon and the surrounding muscles, improve flexibility, and promote proper foot mechanics. Specific exercises may include heel raises, arch strengthening exercises, and calf stretches. It is recommended to perform these exercises under the guidance of a physical therapist to ensure correct form and avoid further injury. The frequency and intensity of exercises may vary based on individual needs and progression.
Incorporating conservative treatments such as physical therapy exercises can help individuals manage pain, reduce inflammation, and promote healing in cases of posterior tibial tendonitis. These non-invasive treatment options are often effective, particularly when implemented early in the course of the condition.

Advanced Treatment Options for Posterior Tibial Tendonitis
Extracorporeal Shockwave Therapy (ESWT)
Extracorporeal Shockwave Therapy (ESWT) is a non-invasive treatment that uses high-energy sound waves to stimulate the healing process in the affected tendon. ESWT has shown promising results in promoting tissue regeneration, reducing pain, and improving function in individuals with posterior tibial tendonitis. The procedure involves the application of shockwaves to the affected area under the guidance of a healthcare professional. ESWT may require multiple sessions for optimal outcomes, and the specific benefits and considerations should be discussed with a healthcare provider.
Platelet-Rich Plasma (PRP) Injections
Platelet-Rich Plasma (PRP) therapy involves using the patient's own blood, processing to concentrate platelets and growth factors, and injecting it into the affected tendon. PRP injections have the potential to enhance the healing process and reduce inflammation in posterior tibial tendonitis. The platelets and growth factors present in the PRP solution can stimulate tissue repair and regeneration. The use of PRP injections for posterior tibial tendonitis should be discussed with a healthcare professional, considering individual circumstances and potential outcomes.

These advanced treatment options, such as extracorporeal shockwave therapy (ESWT), and platelet-rich plasma (PRP) injections, provide additional avenues for managing posterior tibial tendonitis when conservative treatments are insufficient. It is important to consult with a healthcare professional to determine the most suitable approach based on individual needs and the severity of the condition.
Surgical Treatment Options for Posterior Tibial Tendonitis
Indications for Surgical Intervention
Surgical intervention for posterior tibial tendonitis should only be considered in the most serious cases when conservative treatments have failed to alleviate symptoms or when the condition is severe. Indications for surgery may include significant tendon damage, persistent pain, loss of function, and instability of the foot and ankle.
Strategies for Preventing Future Posterior Tibial Tendonitis Episodes
Preventing future episodes of posterior tibial tendonitis is essential for long-term foot health. The following strategies can help reduce the risk of recurrence:
Proper footwear
-
- Choosing appropriate footwear is necessary. Depending on which stage of PTTD you are in. If you are in a more advanced stage, we highly recommend seeing a practitioner as orthotics and more aggressive treatments may be necessary.
Gradual and Appropriate Training and Activity Progression
-
- Avoiding sudden increases in physical activity or training intensity is important to prevent overuse injuries, including posterior tibial tendonitis. Gradually increasing the duration, frequency, and intensity of activities allows the body to adapt and reduce the risk of straining the tendon. It's crucial to listen to the body, recognize signs of fatigue or pain, and adjust training accordingly. If you want a 12-week program for optimum foot health, try our Fit Feet Program, designed by clinicians and tailored to your feet.
Maintaining a Healthy Weight and Lifestyle
-
- Excess body weight puts additional stress on the feet and ankles, increasing the risk of developing or worsening posterior tibial tendonitis. Maintaining a healthy weight through a balanced diet and regular exercise helps reduce the strain on the tendon and promotes overall foot health. Incorporating low-impact exercises, such as swimming or cycling, can be beneficial for maintaining fitness without excessive stress on the feet and ankles.
By implementing these preventive measures and maintaining a proactive approach to foot health, individuals can minimize the risk of future posterior tibial tendonitis episodes and enjoy an active and pain-free lifestyle.
Note: It's essential to consult with a healthcare professional or physical therapist for personalized advice and guidance on rehabilitation exercises and preventive strategies based on individual circumstances. If you would like to see a Gait Happens Clinician online, you can book an appointment here.
Conclusion
In conclusion, posterior tibial tendonitis can significantly impact foot health and mobility, but there are various treatment options available to alleviate symptoms and promote recovery. Throughout this article, we have explored the different treatment approaches for posterior tibial tendonitis, ranging from conservative measures to advanced therapies and surgical interventions.
Conservative treatments, such as rest, ice, compression, elevation, medications, and physical therapy exercises, can effectively reduce pain and inflammation while improving strength and flexibility. Advanced options like extracorporeal shockwave therapy (ESWT), and platelet-rich plasma (PRP) injections offer additional benefits in promoting healing and restoring function.

In some cases, surgical intervention may be necessary, and procedures like tendon debridement and repair or tendon transfer/reconstruction can address severe or persistent cases of posterior tibial tendonitis. Rehabilitation exercises and a structured recovery plan are crucial post-surgery to optimize outcomes and regain optimal foot function.
However, it is important to note that every individual's condition is unique, and seeking professional advice is vital for an accurate diagnosis and personalized treatment plan. A healthcare professional or specialist can assess the severity of your posterior tibial tendonitis, recommend the most appropriate treatment options, and guide you through the recovery process.
Early intervention is key in managing posterior tibial tendonitis effectively. By promptly seeking medical attention, adhering to recommended treatments, and following preventive measures, individuals can achieve successful recovery and reduce the risk of future complications. Preventive strategies like proper footwear selection, gradual training progression, and maintaining a healthy weight and lifestyle contribute to long-term foot health.
Remember, this article serves as an informative guide, but it is essential to consult with a healthcare professional who can provide personalized advice based on your specific condition. By taking proactive steps and working closely with a healthcare team, you can overcome posterior tibial tendonitis, regain foot function, and enjoy an active, pain-free life.
FAQs (Frequently Asked Questions) about Posterior Tibial Tendonitis Treatment
What is posterior tibial tendonitis, and what are the available treatment options?Posterior tibial tendonitis refers to inflammation and irritation of the posterior tibial tendon, causing foot pain and affecting mobility. Treatment options include conservative measures like rest, compression, and elevation, as well as advanced treatments like orthotics, physical therapy, and surgery.
How is posterior tibial tendonitis diagnosed, and what are the recommended treatment approaches?Early diagnosis and prompt treatment are important for posterior tibial tendonitis. Diagnosis is typically made based on a physical examination and sometimes imaging tests. Early detection is key as there are 4 stages of PTTD.
Treatment approaches may include rest, medication for pain and inflammation, physical therapy exercises and stretches, orthotics, extracorporeal shockwave therapy, platelet-rich plasma injections, and surgical options.
Can I treat posterior tibial tendonitis at home?Certain aspects of posterior tibial tendonitis treatment can be managed at home. Following prescribed physical therapy exercises and stretches as part of a home exercise program may also be beneficial. However, it is important to consult with a healthcare professional for an accurate diagnosis and guidance on home treatment.
How long does it take to recover from posterior tibial tendonitis?Recovery time for posterior tibial tendonitis varies depending on the severity of the condition and individual factors. Mild cases may improve within a few weeks with conservative treatment, while more severe cases or those requiring surgery may take several months for a full recovery. Consistent adherence to recommended treatments and rehabilitation exercises can significantly contribute to successful recovery.
Please note that the answers provided here are for informational purposes only and should not replace professional medical advice. It is essential to consult with a healthcare professional for an accurate diagnosis and personalized treatment plan based on your specific condition.
*Please note that the answers provided here are for informational purposes only and should not replace professional medical advice. It is essential to consult with a healthcare professional for an accurate diagnosis and personalized treatment plan based on your specific condition.